
Skin and Rashes
1/3/2022
Skin is an amazing organ. It is our largest organ containing over 19 million cells! Our body is constantly making new skin cells and getting rid of old skin cells. We make and shed over 30-40,000 skin cells every day. The top 18-23 layers of our skin are all dead skin cells. And did you know, just one inch of skin has 650 sweat glands, 20 blood vessels, 60,000 melanocytes (the cells that give your skin color), and 1,000 nerve endings!
Our skin has lots of jobs. Each of the 3 layers have different jobs that help keep our body safe and warm. The top layer, the epidermis, protects your body and gives your skin its color. The thickness of this layer is different depending on the area of your body (thin on your eye lids, thick on the soles of your feet).
The next layer is the dermis. The dermis makes sweat, helps you feel things, grows hair, and makes oil. The bottom layer is the subcutaneous fat. This layer attaches your skin to muscle and bones, helps hold the blood vessels and nerve cells, control body temperature, and stores fat that pads and protects your body.
The top layer of skin is the layer we see and the layer where we can see rashes. And children, from the day they are born, can get rashes and have skin issues. Today we are going to learn about common childhood skin conditions and rashes. Links to mentioned over the counter treatments can be found here.
Skin Conditions
Children are more likely to have skin issues. This is because their skin is thinner, more delicate, and can lose moisture more easily than adults.
Dry Skin
Dry skin is a common occurrence in younger children. Dry skin can be itchy and uncomfortable. Dry skin may appear red and chapped or scaly. It may feel rough to the touch.
Treatment
If your child has dry skin, the goal is to add moisture. If your child has dry skin keep baths or showers short, with a goal of being under 10 minutes, and keep the bath water lukewarm. Avoid scented soaps, bubble baths, and foaming soaps. After bathing, pat the skin dry but don’t fully dry the skin. When the skin is still slightly damp, apply moisturizers.
There are three types of moisturizers. Ointments have the most oils and include products like Vaseline and Aquaphor. Creams have a lotion like texture but have more oil in them then lotions. Lotions are very light and contain the least amount of oil.
In addition to good skin care, try adding moisture to your child’s environment by running a cool mist humidifier in their bedroom. Good skin care also includes avoiding scented products and detergents.
Eczema
Eczema is a chronic skin condition. Eczema causes the skin to be dry, scaly and red. In babies, the scalp, face, cheeks, forehead, and around the mouth can be heavily affected. In older children, the elbow creases, back of knees, neck, and around the eyes are commonly affected areas.
Eczema is caused by problems with the skin barrier. It is believed that eczema prone skin does not have enough filaggrin protein in the outer layer. This causes the skin to have a hard time holding in water as well as a hard time keeping irritants and bacteria out. It can run in families. It can also be caused by allergic conditions such as asthma, seasonal allergies, and food allergies.
Eczema can flare up during cold weather, when the air is dry, by pressurized air on planes, when overheated, or due to excessive sweat. It can also be triggered by fragrances, hormones, insect bites, allergies such as pollen, dust mites, or pet dander, tobacco smoke, and synthetic fabrics. Avoiding the listed triggers can help prevent eczema flares.
Children with eczema should be dressed in soft breathable fabrics. Laundry detergent should be mild and fragrance-free. Nails should be kept short so they cannot scratch themselves while itching their eczema. Scratching and open the skin and result in skin infections.
Treatment
The goal of treating eczema is to improve the skin barrier. A strong skin barrier keeps the skin hydrated, reduces flares, and reduces itching. Baths or showers should be kept short, and the water kept lukewarm. A gentle, unscented cleanser that does not foam should be used. Avoid harsh scrubbing or using bubble baths as these exacerbate eczema. After bathing, pat the skin dry but leave it damp. Moisturize with a fragrance-free cream or ointment daily. Lotions may not have enough oil content to moisturize skin with eczema. Daily skin care, not just attention during times of flares or when skin feels dry, is important to prevent exacerbations or eczema flares.
Moderate or severe eczema may require medication to help bring down inflammation and heal the skin. Topical steroids, such as hydrocortisone, can be used twice a day for a few days during a flare. If over the counter steroids are not improving your child’s eczema, they may need a prescription strength topical steroid. Steroids should not be used on delicate skin such as on the face or around the eyes. There are prescription non-steroidal creams that can be helpful at addressing eczema in these areas.
Bleach baths are recommended for children who have severe eczema or are prone to skin infections. A bleach bath can be done 2 to 3 times a week. As scary as this sounds, it is safe to do as the water in a bleach bath will be the same as a chlorinated pool. For a full bathtub of water, you should add ½ cup of bleach. For a full infant tub, add 2 tablespoons of bleach. The bleach should not be the splash free version or contain fragrance. A child should soak in a bleach bath for 10 to 15 minutes. It is safe for this water to be on their face and scalp. At the end of the bleach bath, rinse them off with plain water and apply moisturizers as described above.
Another option for more severe eczema is using wet wrap treatments. Wet wrap treatments are done after bathing and after applying topical medications and moisturizers. To do a wet wrap treatment, soak a pair of PJs, soft clothing, or onesie in warm water. Wring out the clothing until it is damp, not soaking, and put it on your child. Wrap them in a warm blanket or increase the room temperature so it is warm. Your child should keep the wet clothing on for 30 minutes, but it can be kept on overnight if tolerated. When you take the wet clothing off, reapply moisturizer.
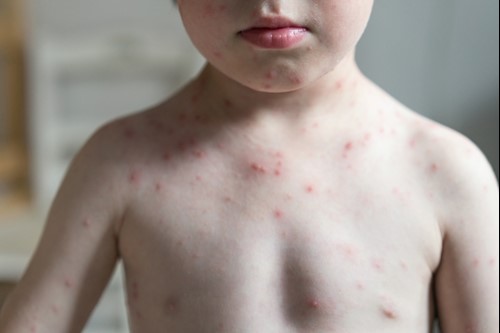

Infectious Skin Conditions
Viral
Warts
Warts are caused by viruses that enter small openings in the skin. Warts are tiny firm bumps on the skin. They can be yellow, tan, black, brown, or gray and may contain black dots (these are clotted blood vessels). They tend to occur on hands, knees, feet, and toes.
Warts will self-resolve after several months to a year. Treatment is available for warts if they are painful or annoying. Treatment for warts includes over-the-counter medications that contain salicylic acid, using duct tape (this really works), or the warts may require treatment in office or with a dermatologist.
Molluscum Contagiosum
Molluscum contagiosum is a specific type of viral wart. Molluscum appears as small bumps that have tiny dimples or “belly buttons” in the center. The warts are usually seen on the trunk, arms, and legs often in areas where skin touches. The rash is self-limited and should resolve on its own in 6-12 months.
The rash can be itchy as it can have small patches of eczema around each wart. Itching can cause the warts to spread or become infected. If the warts are itchy, hydrocortisone can be applied to reduce itching.
Molluscum are contagious. Do not share towels, bedding or clothing that is unwashed to prevent the spread to other household members.
Roseola
Roseola is one of the most common viral infections we see in babies and young children under the age of 2. This infection occurs 7 to 14 days after exposure.
Roseola starts with 3 to 7 days of a high fever. The fever may be accompanied by cold symptoms including a runny nose and cough. Once the fever breaks, a raised spotted pink rash develops on the trunk and sometimes the face, arms, and legs. Roseola requires no treatment other than comfort measure during the fever stage of the roseola virus.
Fifth's Disease
Fifth’s disease is a rash caused by Parvovirus B19. This virus causes bright red “slapped” cheeks and a lacy rash on the arms and legs. This rash may be itchy, and you may also have cold-like symptoms. The rash develops 4 to 21 days after being exposed to the virus. The virus is most contagious before the rash occurs. This is a virus you usually only get once in your life. Fifth’s disease will self-resolve without treatment.
Fifth’s disease can be problematic to pregnant women who have not been previously infected. The virus can cause issues to a developing fetus. If a person has Fifth’s disease and they encounter a pregnant woman during the contagious period, they should alert that person who can be tested to see if they have antibodies to Parvovirus B19.
Bacterial
Impetigo
Impetigo is a bacterial skin infection. It is commonly seen during hot, humid weather but can occur at any time. The rash appears as fluid filled blisters that sometimes ooze and develop yellow or honey-colored scabs. If only one blister or scab is present, topical antibiotics may be adequate. If the rash is spreading, oral antibiotics may be necessary.
Impetigo is contagious. Make sure the rash is covered and your child avoids scratching. A child should remain out of school or daycare until the rash has been treated with antibiotics for 24 hours.
Scarlet Fever
Scarlet fever, or scarlatina, is what we call the rash from strep throat. The rash is usually found on the trunk but can also be found on the arms and legs. Scarlet fever may cause the face to be red, but the skin around the mouth may appear pale. The rash on the trunk is generally fine, red, and raised. It feels like sandpaper. As the rash progresses, it may leave peeling skin. The treatment is oral antibiotics to treat the strep throat.
Hot Tub Rash
Hot tub rash, or folliculitis, is a rash resulting from bacteria in unclean pools or hot tubs or from wearing a bathing suit that is damp. The bacteria irritate hair follicles on the body and cause the hair follicles to become infected. The rash is generally small red pimples that can be anywhere but most often are noted on the skin under a bathing suit. The rash usually emerges 12-48 hours after exposure to the pool or hot tub.
Despite being a bacterial rash, this rash rarely needs treatment with antibiotics. It often clears on its own though you can use hydrocortisone cream and calamine lotion to help with any itching.
Fungal
Ringworm
Ringworm is a fungal infection like athlete’s foot or jock itch. Ringworm results in a rash that is circular, has red raised or scaly edges, and has a round smooth center. It can occur on the scalp or body.
Ringworm can spread quickly especially in warm, damp conditions. It often spreads quickly in athletes using shared equipment or mats. Disinfecting equipment and mats can help prevent the spread.
Ringworm is treated with anti-fungal cream for 3 weeks. The rash can take over a week to start to resolve. It is contagious until 72 hours after treatment is initiated. Until the 72 hours is completed, the rash should be covered if possible and athletes should not participate in sports where it may easily spread.
Reactive or Inflammatory Skin Conditions
Hives
Hives, or urticaria, is a reactive rash that can have many causes. The rash may occur as a reaction to food, medication, or additives to food. Hives also can occur due to heat, cold, exercise, sunlight, stress, and underlying illness. Viruses and bacterial infections can cause hives. Hives also occur, idiopathically, meaning we cannot identify the cause.
Hives are pink or red bumps or welts. They can be small or large. Sometimes they look like there is bruising under the hives. Depending on the cause, hives can last for hours or for days. Some people suffer from chronic hives.
Hives are treated with antihistamines including Benadryl, Zyrtec, or Allegra (Claritin is not effective for hives) to reduce the itching. Depending on the cause and duration of the hives, additional treatment and evaluation may be necessary.
Also, for hives due to bacterial illness, such as strep throat or mycoplasma pneumonia, addressing and treating the underlying cause will treat the hives.
For hives caused by environmental factors, avoiding those triggers, such as offending foods and ingredients, stress, temperature extremes, and sunlight, will reduce urticaria outbreaks.
Heat Rash
Heat rash is a reaction to heat. Heat rash occurs in babies and young children when their sweat glands are blocked. It results in rash of small pink or red bumps usually in covered areas. Most often the rash will appear on their upper back, neck, and folds such as elbows, armpits, thighs. The treatment goal for heat rash is to keep skin cool and dry. Remove layers or keep skin bare if it is very hot. Do not apply any lotions or moisturizers as they will continue to block the sweat glands.
Poison Ivy
Poison ivy or other plant-based rashes occur due to exposure to a sticky oil called urushiol. Urushiol causes an itchy and burning rash in areas that the oil has touched. The rash may be in lines or patches and can have oily appearing bumps or blisters and may even have areas that weep clear fluid. The rash may also cause localized swelling. Poison ivy is not contagious.
If your child comes across poison ivy or other plants that cause rashes, wash the areas with soap and water for 10 minutes. Make sure to trim fingernails and clean under nails as any oil present under the nails can continue to spread the rash. Additionally, all clothing should be washed in hot water and soap.
Topical lotions such as calamine lotion and hydrocortisone cream can help soothe the rash and treat the rash. Oral antihistamines such as Benadryl or Zyrtec can help reduce itching. It is important to reduce the desire to itch as itching can cause the rash to become infected.
If the poison ivy is severe, on the face or groin area, or not responding to over-the-counter treatments, oral steroids may be necessary.



Insect Bites
Insect bites are the most common reactive rash that we will see on our children. Bites can be from mosquitos, fire ants, bees or wasps, and other biting insects. These rashes cause itching and minor discomfort. Bee or wasp stings can also cause anaphylaxis.
Prevention is key. Avoid scented soaps and shampoos and avoid wearing bright clothing as these attract insects. Avoid playing around stagnant water or blooming flowers. If you will be outdoors, cover your skin with light clothing and use insect repellent.
If your child is stung, remove the stinger immediately. Clean the skin, apply ice for 10 minutes, then apply calamine lotion or hydrocortisone. If your child is bit by an insect that causes welts and itching, you can apply ice immediately and hydrocortisone, calamine lotion, or Benadryl cream to relieve itching. Preventing itching will help to reduce the chance of the bite becoming infected.
Children tend to have more “robust” reactions to insects than adults. This is because their immune system is immature and has had less exposure to insect bites. Some people who have “Skeeter Syndrome” will always have big reactions to bites. A child who has a bite on the foot can have whole foot swelling. A child with a bite above the eye can have an eye that is so swollen that the eye cannot open. These reactions are normal but may require oral Benadryl to help stop the reaction and bring down swelling.
Swimmer's Itch
Swimmer’s Itch, also called Duck Rash, is a rash that occurs after being in lakes, ponds, or oceans. The rash is the result of microscopic parasites found in shallow waters near the shore. The parasites burrow into the skin and cause inflammation. Swimmer’s itch is a raised rash of red spots that occasionally turn into welts or blisters. The rash is usually found on areas NOT covered by bathing suits.
Swimmer’s itch can be prevented by not swimming in marshy areas, by avoiding areas that have a lot of ducks present, and swimming in deeper waters. You can also prevent swimmer’s itchy by showering or vigorously rubbing skin off with a towel immediately after getting out of the water. This helps wash or rub off any parasites that are on your skin.
Swimmer’s itch is treated with calamine lotion, oatmeal baths, or Epsom salt baths. You can also use hydrocortisone creams.

Juvenile Plantar Dermatosis
Juvenile plantar dermatosis is a rash that is often mistaken for athlete’s foot. It is a red rash on the feet. It can be red and smooth, or the skin can appear cracked or scaly. It is different than athlete’s foot because it can be on areas that are not typical to athlete’s foot including the soles of the feet. It is often found on the balls of the feet and the bottom of the big toe.
This rash is the result of feet getting wet then drying out quickly repeatedly. Because children’s feet have more sweat glands then adults, their feet easily get wet. Breathable footwear and thick absorbent socks can help prevent Juvenile Plantar Dermatosis. This rash is treated with steroid creams.
Pityriasis Rosea
Pityriasis rosea is an inflammatory skin disorder with no identified cause. It generally occurs during adolescence or young adulthood. The rash has two phases. In the first phase a person develops a large pink spot on their chest, back, arms, or legs. This is called a herald patch. It looks similar to ringworm and can be misdiagnosed as such. The second phase of the rash, occurring 1 to 2 weeks later, results in small pink oval areas that look similar to small patches of eczema. The rash is often in a Christmas tree like shape on the trunk. It very rarely affects the face. The rash may be mildly itchy. A person may also feel slightly fatigued during this time.
The rash lasts 3 to 9 weeks and resolves without treatment. Treatment should be aimed at comfort. Rest and topical lotions that decrease itching can be helpful.
Intertrigo
Intertrigo is an inflammatory rash that occurs in skin folds and warm wet places. Often babies will get this rash in their neck or thigh folds or in the diaper area. To prevent intertrigo, keep folds dry and clean. After feeds make sure to clean, your child’s neck to remove any breastmilk, formula, or food that may has become trapped. Frequent diaper changes can prevent intertrigo in the diaper area. During diaper changes make sure to allow time for the skin and folds to dry or actively dry these areas.
Intertrigo rashes can become infected with yeast or bacteria. This may require anti-fungal creams and topic or oral antibiotics.
Diaper Rashes
Irritant
An irritant diaper rash is due to moisture, dyes or certain brands of diapers, scented wipes, or something in the diaper (such as loose stool) irritates the skin. It may look like red bumps or spots. It can have welts and may open, have sores, or bleed. Open or cracked areas increase the risk of secondary infection.
Treatment includes frequent diaper changes and diaper cream. For severe diaper rashes the following works very well:
- Dry the skin thoroughly
- Apply a thin layer of Maalox (the liquid antacid) to the buttocks using a cotton round and allow it to dry
- Apply a thick area of a zinc-based diaper dream (my favorite is Desitin Max because it has 40% zinc)
- Apply a thick layer of Vaseline or Aquaphor to coat.
Candidiasis
Candidiasis, or yeast, diaper rashes is due to excessive growth of yeast in the diaper area. The rash will be red and inflamed. It may look “beefy” and may have a white scaly outer layer. Sometimes the rash will have blisters or small red bumps or spots around the larger rash.
Yeast diaper rashes are treated with anti-fungal creams such as clotrimazole cream or nystatin cream or ointment. Allowing skin to dry out by having 5-10 minutes of diaper free time can also help treat and prevent this type of rash.
Bacterial
Bacterial diaper rashes cause red, swollen, and inflamed skin. There may be large hard lumps or pimples noted. Some babies may have a fever, but many do not. This rash may be the result of an infection due to openings in the skin. This rash is treated with topical or oral antibiotics depending on the severity of the rash. You may also use a zinc-based diaper cream to sooth any open or sore areas.
The rashes discussed above Is not an all-encompassing list but some of the more frequent rashes we see in children. If your child has a rash that is not responding to over the counter treatment, please do not hesitate to bring them in for an evaluation and treatment plan.
Children’s Health Care of Newburyport, Massachusetts and Haverhill, Massachusetts is a pediatric healthcare practice providing care for families across the North Shore, Merrimack Valley, southern New Hampshire, and the Seacoast regions. The Children’s Health Care team includes pediatricians and pediatric nurse practitioners who provide comprehensive pediatric health care for children, including newborns, toddlers, school aged children, adolescents, and young adults. Our child-centered and family-focused approach covers preventative and urgent care, immunizations, and specialist referrals. Our services include an on-site pediatric nutritionist, special needs care coordinator, and social workers. We also have walk-in appointments available at all of our locations for acute sick visits. Please visit chcmass.com where you will find information about our pediatric doctors, nurse practitioners, as well as our hours and services.
Disclaimer: this health information is for educational purposes only. You, the reader, assume full responsibility for how you choose to use it.








