
Headaches
3/14/2022
Headaches are pain or discomfort in the head. This pain can occur from the forehead to the neck. Over 90% of children have experienced a headache by age 18. There are many types of headaches, many triggers for headaches, and different treatments for headaches.
ACUTE HEADACHES
Acute headaches are suddenly occurring discomfort of pain that gets worse quickly.
ACUTE HEADACHE TYPES
Acute headaches can be caused by viruses, hunger, sinus infection, meningitis, or be a common headache.
Viral
Viral headaches may be caused the virus or may occur due to the fever your body raises to fight the virus. These headaches can last for a few days but often are relieved by acetaminophen or ibuprofen.
Hunger or Dehydration
Hunger is a frequent cause of headache with over 30% of people having headaches due to hunger. Food fixes these types of headaches, but it can take up to 30 minutes after eating to relieve the headache.
Dehydration causes 1 in 10 headaches in kids. This includes even mild dehydration from not consuming enough liquids, especially water. Children are more susceptible to dehydration than adults due to higher body surface area. Boys are more likely than girls to become dehydrated.
Sinusitis
Frontal sinus infections can cause headache. This pain will be felt just above or below the eyebrows and will be accompanied by upper respiratory infection symptoms that have been present for over a week and are worsening. Children under 10 do not have fully formed frontal sinuses, so these headaches are usually not seen before age 10.
Meningitis
Meningitis is the most dangerous of acute headaches. Meningitis is an infection of the membrane that surrounds the brain and spinal cord. A person will also have a stiff neck, fever, and possibly confusion, irritability, or lethargy. This is a medical emergency.
Common Headaches
Common headaches are acute headaches caused by a trigger. These triggers can include
- Exercise
- Bright sunlight
- Playing a wind instrument
- Severe coughing
- Chewing gum

RECURRENT HEADACHES
Recurrent headaches are headaches that occur more than once such as tension headaches or migraines.
CHRONIC HEADACHE TYPES
Tension Headache
Tension headaches are the most common headaches we see in people. Tension headaches cause a constant, dull, or achy pain in the forehead or both sides of the head. A person may feel a sensation of tightness or a band around their head. They may also have sore neck muscles and fatigue.
Tension headaches can occur due to holding a position to long such as when reading or using a computer. It can also be a reaction to stress or worry. It can also result from TMJ or jaw clenching.
These types of headaches generally happen later in the day and have a slow onset
Chronic Daily Headache
Chronic daily headaches are when tension headaches occur more than 15 times a month. These headaches are particularly upsetting for patients and parents due to the frequency of the headaches. They can also be hard to manage because the medications that treat the headaches, ibuprofen, acetaminophen, and naproxen, can actually cause the headaches if used too frequently.
To combat chronic daily headaches, a person much find their trigger or exacerbations and work to minimize those.
Cluster Headache
Cluster headaches are uncommon in children, particularly those under 10 years of age. Cluster headaches occur in episodes of 5 or more headaches in one day or every other day. They cause sharp stabbing pain behind an eye. It may also cause tearing, congestion, and runny nose on the side of face feeling pain. The episode usually last less than 3 hours.
Vision Strain Headache
A vision strain headache is not related to a vision issue (which can cause headaches) but to straining to see the blackboard. It presents like a tension type headache. It is NOT resolved by glasses.
School Avoidance Headache
School avoidance headaches occur on the mornings of school days. These headaches come with REAL PAIN. They are exacerbated by stress and often occur in children with low pain thresholds.
MIGRAINE HEADACHES
A migraine headache is one that is severe, painful, and throbbing. In adults it is felt on one side of the head but can be on one side or bilateral in children. Migraines come on suddenly and can be accompanied by nausea or vomiting. Over 80% of children will have nausea, vomiting, or abdominal pain with migraines. Lights and sound can make migraines worse. Some children will feel a tingling sensation or see spots.
Pediatric Criteria and Diagnosis
Pediatric criteria to be diagnosed with migraines is different than adults. To be diagnosed a child must have 5 or more headaches that have lasted 2 to 72 hours. These headaches cannot be caused by anything else including medication overuse. A child must have 2 or more of the following symptoms:
- Pain is located bilaterally
- Pulsating quality to the headache
- Moderate to severe pain
- Headache worsens with activity
They must also have one of the following symptoms:
- Nausea
- Vomiting
- Photophobia
- Phonophobia
If a child has migraines, they should be seen by a neurologist or headache medicine specialist to confirm diagnosis and rule out other causes. Adolescents may be able to be managed by their primary care provider if they only need recovery treatments.
Migraine Causes
It was previously thought migraines were due to dilated blood vessels, but newer research shows it may be related to brain chemical or electrical signals. Migraines affect over 39 million people. Of children aged 5-15, 10% have had a migraine. This increases to 28% for children up to age 18. Children who were colicky babies are 7 times more likely to have migraines. We also see a high comorbidity with anxiety and depression although they are not sure if one causes the other or vice versa. People with migraines are also more likely to have insomnia, irritable bowel disease, and heart disease including stroke.
Migraines run in families. If one parent has migraines a child has a 50% chance of having migraines. If both parents have migraines, that child has a 90% chance of having migraines. Before puberty, more boys have migraines but this changes after puberty with 7% of boys having migraines and 23% of girls having migraines.
Migraine Phases
Migraines occur in 5 phases:
- Warning phase
- Up to 24 hours before
- Symptoms include tiredness, sore neck, mood changes
- Aura
- Not experienced by all migraine sufferers
- Up to an hour before an attack
- Visual signs such as spots, wavy lines
- Dizziness
- Weakness
- Numbness
- Confusion
- Headache or attack phase
- Severe throbbing pain
- Nausea
- Vomiting
- Resolution
- Sleepy period during/after migraine
- Recovery
- Feeling tired for hours to days after a migraine
Migraine Triggers
Migraine triggers are different for each person but identifying and avoiding a person’s triggers can help reduce the frequency of migraines. Triggers include:
- Irregular sleep schedules including too much or too little sleep
- Changes in stress levels
- Hormones (2-3 days before and into menstruation)
- Exercise
- Skipping meals
- Dehydration
- Food additives such as nitrates found in aged meats and cheeses
- Chocolate
- Citrus fruits
- Red or yellow food dye
- MSG
- Aspartame
- Caffeine
- Spicy foods
- Stormy weather
- Extreme heat or cold
- Bright sunlight/glare
- High humidity
- Dry air
- Screen time
Triggers can be hard to identify but a free application called Migraine Trainer can help children and teens chart potential triggers.

RED FLAG HEADACHES
If your child has headache symptoms that include the below, they may need an urgent headache work up to rule out infection, a brain tumor, or other diagnosis:
- Daily headaches
- Headaches from straining, coughing, sneezing, or when stooling
- Headache with eye pain, confusion, or numbness
- Headaches that continuously get worse or keep returning
- Headaches that wake a child from sleep
- Headache with personality changes
- Headaches with persistent vomiting
- Headaches that improve with vomiting
- Headaches with persistent visual changes
- Headaches described as the worst headache ever
Most parents big fear with headaches is a brain tumor. Over 98% of all children with a brain tumor will have an objective finding on their neurological exam that indicates further work up. This can be determined by a physical exam.
HEADACHE TREATMENT
Headache treatments will depend on the type of headache and the severity of the headache. In order to identify the type of headache your child is having and potential treatment plans, you should help your child keep a headache diary, over the course of a few weeks, with the following information:
- Date and time of onset of headache
- How long did the headache last?
- Where was the pain and how did it feel (sharp, dull, aching?
- Any other symptoms
- What helped the headache (treatments, rest ect)
- What made the headache worse (lights, sound, moving)
- Any specifics from that day (stressors, food, trouble sleeping etc)
Your child may need help figuring out their level of pain. Younger children may need a visual reference point and older children may be able to use a number-based rating system. If your child reports a high level of pain but is playing, eating, and acting normally, they may need to consult a visual reference. This is not usually an accurate pain assessment, so showing pictures of what pain levels look like can result in more accurate pain ratings. One such as the one below can be helpful:
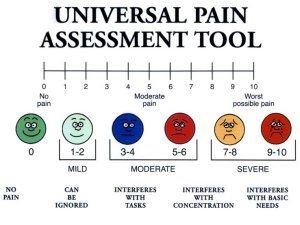
While tracking your child’s headaches, make sure to work on the 4 essential health habits that can help prevent headaches: diet, hydration, exercise, and sleep (see side bar) to see if these improve the frequency and severity of symptoms.
PREVENTION
Diet
A well-balanced diet can help prevent headaches. This includes eating 3 meals and 2-3 snacks a day. Skipping meals may lead to hunger headaches or migraines. Meals and snacks should include a protein, fiber, and fat. Avoid any identified food triggers.
Hydration
To ensure adequate daily hydration, you should have at least 4-6 cups of fluids, more if your body requires it. You may also need more when weather is hot, or you are exercising. Fluids can also be counted via fruits and vegetables.
Exercise
Exercise can trigger some headaches, but overall exercise has been shown to reduce the frequency and severity of headaches, particularly tension headaches. Exercises increases oxygen flow and releases feel good chemicals in your body. Exercise can include yoga, stretching, cardiovascular workouts including walking, running, swimming, and resistance training. The goal is at least 20 minutes, three times a week.
Sleep
Older children and teens need 8-10 hours a sleep at night. Sleep patterns should be consistent meaning bedtime and wake times should stay the same every day. Too much sleep and too little sleep can both contribute to headaches. Screens should be shut off at least 1 hour before bedtime.
ACUTE TREATMENT
Medication
Acute or chronic headaches are often treated the same way including acetaminophen, ibuprofen, or naproxen at the time of headache. A child should have no more than 3 doses a week for non-viral headaches, or they can become dependent on the medications resulting in chronic daily headaches. Narcotics should always be avoided. Viral headaches due to fever should be treated as need to ensure comfort and hydration.
Non-pharmaceutical treatment
Non-pharmacological treatments that have been shown to improved headaches in children in teens include massage, acupuncture, biofeedback, and guided imagery.
Those with chronic daily headaches particularly benefit from behavioral therapy and therapy as well as stress management and biofeedback. It is also essential for these children to manage their headaches through good sleep, proper nutrition, and excellent hydration. School attendance should be mandated as this is frequently a cause of absences.
MIGRAINE TREATMENT
Emergency Treatment aka Abortive Treatment
Abortive treatment is used to help a migraine sufferer improve quickly. The faster a person can take medication at the onset of a migraine, the more likely these medications are to work. Medications include acetaminophen, ibuprofen, naproxen and combination medications of acetaminophen or ibuprofen with aspirin and caffeine. There is also strong evidence that triptans, such as Imitrex or Zomig, work well to stop migraines in teens if taking within 2 hours of headache onset.
If a child has chronic or frequent migraines, they should be seen by a neurologist or headache medicine specialist to confirm diagnosis and rule out other causes. Adolescents may be able to be managed by their primary care provider if they only need recovery treatments.
CHILL is an acronym that lists other helpful emergency treatments.
Cold packs to the back of neck or forehead
Heat to hands and feet to encourage blood flow
Inhale-get away from any strong scents and find cold, fresh air; breathing exercises where you breath in for 8 seconds, hold in 8 seconds, breath out for 8 seconds; also using alternative nostril breathing can help
Liquids-drink 16 ounces of water or a sports drink
Lights out-find a dark room, shade or cover your eyes
Preventative Medication
Preventative medications aim to reduce the frequency or severity of migraines. These medications are prescribed by a neurologist. They include cardiovascular medications, antidepressants, antiseizure medications, and antihistamines.
Research shows that children who have migraines have fewer headaches when treated with amitriptyline (an antidepressant) combined with cognitive behavioral therapy.
Preventative Treatments
Non-pharmaceutical options include cognitive behavioral therapy, acupuncture, and biofeedback.
There is also benefit to vitamin supplementation including Vitamin B2, coenzyme Q10, and magnesium. These can be taken separately but can also be found in combination products such as Migrelief. Vitamin D can also be helpful as many people who have migraines are vitamin D deficient.
If your child is having chronic headaches or migraines that are not improved with diet, sleep, hydration, or exercise; is having any headaches that affect their ability to go to school, socialize, or participate in family or fun activities; or is having any red-flag headache symptoms, please see your primary care provider for an exam and recommendations.
Children’s Health Care of Newburyport, Massachusetts and Haverhill, Massachusetts is a pediatric healthcare practice providing care for families across the North Shore, Merrimack Valley, southern New Hampshire, and the Seacoast regions. The Children’s Health Care team includes pediatricians and pediatric nurse practitioners who provide comprehensive pediatric health care for children, including newborns, toddlers, school aged children, adolescents, and young adults. Our child-centered and family-focused approach covers preventative and urgent care, immunizations, and specialist referrals. Our services include an on-site pediatric nutritionist, special needs care coordinator, and social workers. We also have walk-in appointments available at all of our locations for acute sick visits. Please visit chcmass.com where you will find information about our pediatric doctors, nurse practitioners, as well as our hours and services.
Disclaimer: this health information is for educational purposes only. You, the reader, assume full responsibility for how you choose to use it.








